Before the first neonatal intensive care unit opened in the United States in 1965, premature birth was effectively a death sentence.
Advancements made in neonatology (the care of premature infants) since that time border on the miraculous. In 2017, the National Institutes of Health Maternal-Fetal Medicine Research Network reported a 98 percent rate of survival among infants born at twenty-eight weeks and 88 percent survival for infants born at twenty-five weeks.
In spite of these advances, premature birth remains one of the most common causes of pediatric health complications in the United States. Prematurity affected 10 percent of all US pregnancies in 2019 alone. One in three infants who die in the United States dies because of prematurity; half of all cases of cerebral palsy are attributable to preterm birth. While neonatal intensive care (NIC) has improved drastically in the last twenty-five years, premature infants remain at high risk for chronic lung disease, feeding difficulties, and developmental delay.
There are a multitude of causes for these complications, but one of the most important is the premature arrest of lung development. In the womb, infants receive oxygen from the umbilical cord, and fetal blood flow is shunted away from the unexpanded lungs. In order for these infants to survive premature birth, neonatologists must open and expand the infants’ lungs with high-pressure mechanical ventilation. This intervention allows the premature infant to survive, but also leaves behind significant lung damage that can persist into adolescence or even adulthood. Some of these former premature infants have even required lung transplants as adults.
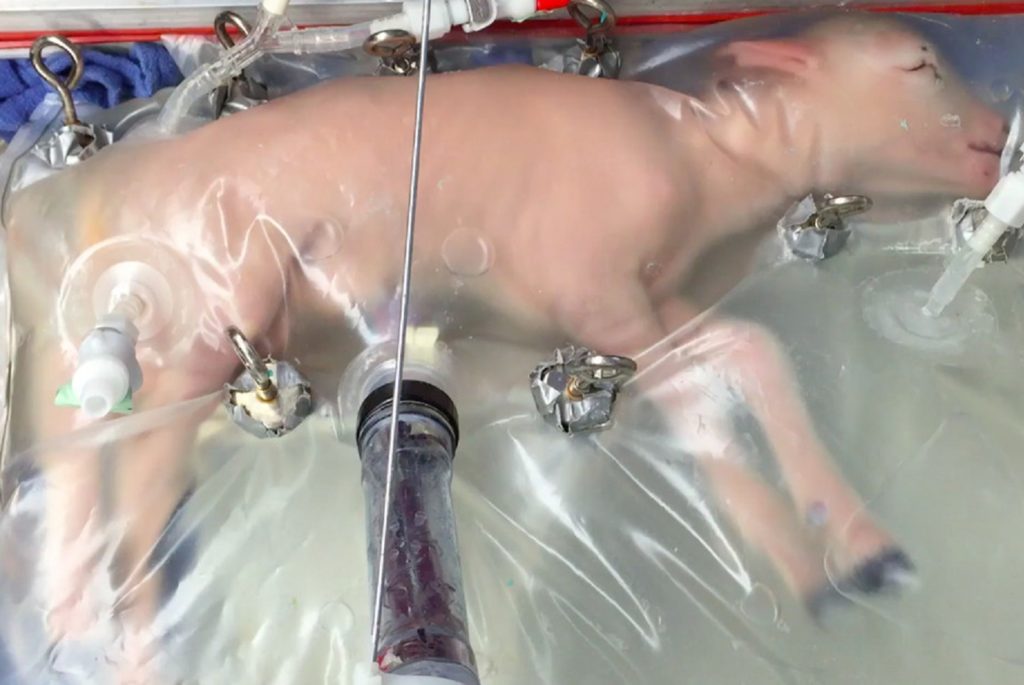
In 2017, researchers at the Children’s Hospital of Philadelphia reported a possible remedy for these premature infants: an artificial womb dubbed the “Biobag.” Fetal lambs born at the equivalent of twenty-three to twenty-five weeks’ gestation for a human infant were transferred to a Biobag and supplied with oxygen and nutrition via the umbilical cord, remaining there for up to four weeks. The fetal lambs that emerged from the Biobag had normal lung function and neurodevelopment compared to age-matched controls. Subsequent studies have confirmed the absence of brain ischemia or injury and demonstrated normal intestinal development in these fetal lambs. While human trials of the Biobag remain years away, these studies indicate that artificial wombs are a realistic possibility for the future of neonatology.
Start your day with Public Discourse
Sign up and get our daily essays sent straight to your inbox.From a Right Not to Gestate to a Right to Kill a Fetus
The ability to maintain fetal physiology outside the womb would cause a massive paradigm shift in our clinical practice. Under current guidance, resuscitating an infant born at less than twenty-five weeks’ gestation is done only with parental request and informed consent. Before twenty-two weeks’ gestation, resuscitation is usually not performed, even if requested by the parents. The Biobag would provide a potent alternative to traditional NIC for these patients and parents.
The implications of these studies have not been lost on medical ethicists. (For a taste of the current ethics literature, you can read the entire special issue the journal Bioethics dedicated to the “Ethics of Ectogestation.”) Philosophers and ethicists have examined numerous issues raised by the development of artificial womb technology (AWT), the most pressing of which has been AWT’s potential impact on abortion rights.
Traditionally, arguments for the right to an abortion in the United States have been grounded in a woman’s right to stop gestating, not a right to end the life of a fetus. Harvard Law Professor Glenn Cohen rightly noted that, if a fetus has reached viability and AWT is available, the argument for the right to an abortion evolves from a right not to gestate and becomes a right to kill the fetus directly—a “much harder sell legally and politically.”
Unfortunately, the medical ethics community has not heeded Professor Cohen’s warning. Some have defended a right to the death of the fetus based on, variously, a right not to be a biological parent, a right to genetic privacy, and property rights. Others have argued that the advent of AWT requires creating a third status of being, conceptually between fetus (in the womb of the mother) and neonate (newborn baby independent of its mother’s body).
Infants occupying this in-between status—what Elizabeth Romanis calls “gestatelings”—would have more rights than a fetus in the natural womb but fewer rights than neonates receiving traditional NIC. In her view, infants in an artificial womb lack an “independent capacity for life,” but are also no longer dependent on the maternal body for survival. Therefore, the “gestateling” is “neither a fetus nor a baby, and the ethical tethers associated with these terms could perpetuate misunderstanding and confusion.” Romanis posits that birth is no longer a sufficiently bright line for establishing personhood.
In a more nuanced argument, the noted Dutch philosopher Elseljin Kingma and Suki Finn proposed moving from the traditional “fetal container model” of pregnancy to a “parthood view” of pregnancy, in which the “embryo/fetus are a proper part of the pregnant organism, like organs, tissue, blood, or any other body part.” As we described above, fetal physiology and circulation in the womb are distinct from those of newborns outside the womb. An infant’s first breath causes a rapid shift away from fetal circulation and oxygenation (dependent on the mother’s circulation) to independent breathing outside the womb (gas ventilation via the lungs). Like Romanis, Kingma and Finn distinguish between fetuses, gestatelings, and neonates, but do so on the basis of the Biobag’s retained fetal physiology:
Gestatelings are treated as if they had never been born, not in the sense that they haven’t left the maternal body—for they have—but in the sense that they haven’t undergone the transition from a fetal physiology to a neonatal physiology. Thus they are only “born” in the sense that they have changed location from inside to outside the maternal body, i.e. “born-by-location-change.” But they are not “born” in the sense that they have changed their physiology from fetus to neonate, i.e. “born-by-physiology-change.”
Kingma and Finn achieve the same end as Romanis by different means: namely, classifying AWT and Biobags as categorically different from traditional NIC. Whereas Romanis makes these distinctions on the vague basis of the infants’ “capacity for life,” Kingma and Finn explicitly tie their argument to the Biobag’s maintenance of fetal circulation and oxygenation.
Artificial Wombs Are Neonatal Care; The Beings They Contain Are Human Infants
The real question is, why do Romanis, Kingma, and Finn feel compelled to make distinctions between AWT and traditional NIC? The goal of AWT and traditional NIC is the same: to improve survival and quality of life for premature infants. AWT would be better for the simple reason that it more closely resembles the natural womb while avoiding lung damage due to mechanical ventilation.
Fortunately, they acknowledge the proverbial elephant in the room: if stopping gestation no longer inevitably entails the death of a fetus, then the entire landscape of abortion rights and jurisprudence has fundamentally changed. For this reason, Romanis, Kingma, and others find it imperative to make a categorical distinction between traditional NIC and AWT. Romanis, Kingma, and Finn all studiously avoid addressing whether making this distinction would allow for the termination of an “artificial pregnancy” in an artificial womb.
As we argued recently in the Journal of Medical Ethics, it is crucially important that AWT, like the Biobag, be properly understood as a natural progression of traditional NIC. All medical care provided to premature infants seeks to mimic the physiology and physical environment of the womb to some degree. Doing this in a safer, more effective manner should neither negate the rights and privileges of these infants nor call their moral status as human beings into question. The fact that professors of philosophy and ethics are doing so in peer-reviewed journals is cause for alarm. It will fall to clinicians, policymakers, and the general public to proactively defend the children cared for with AWT should the Biobag move to human trials. We must do so if we hope to prevent another infringement of ideology into clinical care. Put succinctly, we should “follow the science.”
If stopping gestation no longer inevitably entails the death of a fetus, then the entire landscape of abortion rights and jurisprudence has fundamentally changed.
Ending Gestation No Longer Requires the Death of the Fetus
The ongoing debate over the proper categorization of AWT, though currently relegated to the wilds of academic journals, presents a unique opportunity for unity among pro-life and traditional pro-choice advocates. Defending AWT as NIC has no impact on the argument for the right not to be a gestational parent, particularly when the majority of states limit abortion after viability. The authors of the original Biobag trials explicitly state that the Biobag is not intended to alter the current threshold of viability. Defending AWT as NIC serves pro-life interests by offering a more effective rescue for peri-viable pregnancies that threaten the life of the mother. At the same time, refusing to make an arbitrary distinction between AWT and NIC preserves the “my body, my choice” defense of ending gestation without necessitating a right to the death of the fetus.
Like all medical advancement, AWT forces us to confront the tension between what we can do and what we ought to do. Academicians in bioethics have already begun to try to shape the narrative, and we should not be naïve and ignore the ideas taking hold at a distance. If the Biobag proceeds to human trials, it will still be possible to terminate the premature infant within. The current ethics literature indicates that many academics are prepared to defend this action on the grounds of parental autonomy. Whether these views are embraced by the medical academies or the general public remains to be seen.
A century ago, the fashionable philosophy du jour among academics was eugenics. G. K. Chesterton, clearly seeing the danger of academic discussion spilling over into the public conscience, published Eugenics and Other Evils in 1922. As the medical community prepares to cross a new frontier with the introduction of artificial womb technology, Chesterton’s prescient warning is worth revisiting:
The wisest thing in the world is to cry out before you are hurt. It is no good to cry out after you are hurt; especially after you are mortally hurt. . . . It is no answer to say, with a distant optimism, that the scheme is only in the air. A blow from a hatchet can only be parried while it is in the air.