Decisions about how to care for a terminally ill person are fraught with difficulty. Not every disease can be cured; not every condition has a suitable remedy. At some point, medicine limps, and health cannot be restored. When we reach these limits, we often wonder what we should do. Do we forgo treatment, accepting the inevitability of death? Do we withdraw extraordinary means of life support, recognizing that doing so will likely hasten death? And what if withdrawing treatments fails to bring an immediate end to the patient’s life? What if he lingers? What if he suffers? Wouldn’t it be better if we could find a way to ensure a peaceful death, a death without pain or suffering?
These are the kinds of questions that Gary Comstock raises in his recent contribution to The Stone, a public forum for contemporary philosophers to discuss timely and contentious issues. In his essay, “You Should Not Have Let Your Baby Die,” Comstock walks us through the difficult days following the birth of his son, Sam. Diagnosed with trisomy 18 and a host of associated anomalies, Sam’s prognosis was bleak. Comstock describes in vivid detail what it was like to learn about Sam’s condition and how his family thought through the complexities of his care. He describes the decision to remove Sam from a ventilator. And he tells of the depth of his sorrow as he watched his son die—a death that took far too long and that was accompanied by visible signs of pain and suffering.
Comstock narrates this story, in part, to defend the practice of active euthanasia for children who are suffering from terminal conditions. Toward this end, he describes his own intellectual conversion. He describes the comfort he took, in the midst of his and his wife’s experience making decisions concerning Sam’s care, in the fact that the decision to remove the ventilator was not the same thing as killing his son. There is a moral difference between killing one’s child and letting him die if extraordinary medical care proves futile or burdensome. But Comstock no longer takes comfort in this distinction. In fact, he now believes that it would have been morally better to have killed his son rather than to let him languish. He concludes: “For years you repress the thought. Then, early one morning, remembering again those last minutes, you realize that the repugnant has become reasonable. The unthinkable has become the right, the good. Painlessly. Quickly. With the assistance of a trained physician.”
For Comstock, circumstances like the ones his family faced show why active euthanasia is a moral good. If the goal of removing treatment is to facilitate death, it is heartless at best (and cruel at worst) to allow a person to linger in pain. So, what other options are there? Physicians have the technical capacity to facilitate a quick, painless death. And if one has already made the choice to end a person’s life, failing to employ these means to bring about a painless death is either irrational, or morally wrong, or morally evil.
Start your day with Public Discourse
Sign up and get our daily essays sent straight to your inbox.Comstock’s essay is deeply moving and his reasoning is subtle. There is much to say about the implicit argument he makes in defense of active euthanasia. Some will rightly interrogate his views on the value of human life, especially the value of those whose lives are marked by disability. Others will rightly question his understanding of the nature and purposes of the craft of medicine. Others will raise legitimate concerns about what his reasoning presupposes concerning the moral relationship between a parent and his children. Still others will explore Comstock’s unchecked assumptions about the kinds of good that can be realized in accompanying those who are profoundly ill as they die. Finally, others will raise concerns about Comstock’s failure to attend to the distinction between an act (or omission) whose goal is to bring about death and an act (or omission) one knows will likely hasten death but in which there is no intent to end the patient’s life. All of these are important and crucial lines of response to Comstock’s essay, but I want to leave them to one side in order to focus attention elsewhere.
In many ways, Comstock and I share a common experience, a common sorrow. I think I have some idea of the depths of felt despair and anguish he has experienced. Like Comstock, I had a son who was diagnosed with trisomy 18 and a host of related anomalies. Our son was also named Sam. And he took his final breaths as I held him in my arms. I continue to experience the difficulty of integrating this loss into my life. Finally, Comstock and I share a common vocation: we are both professors of philosophy.
But we hold very different views on the ethics of end-of-life care for terminally ill children. Comstock asserts that the medical community offers limited options to families in need. He would ask physicians to put their abilities to use in ending the lives of children who are dying. But what he fails to say is that there are other options. We don’t have to choose between allowing a person to die a painful, tortuous death and facilitating a quick, painless passing. There is an alternative.
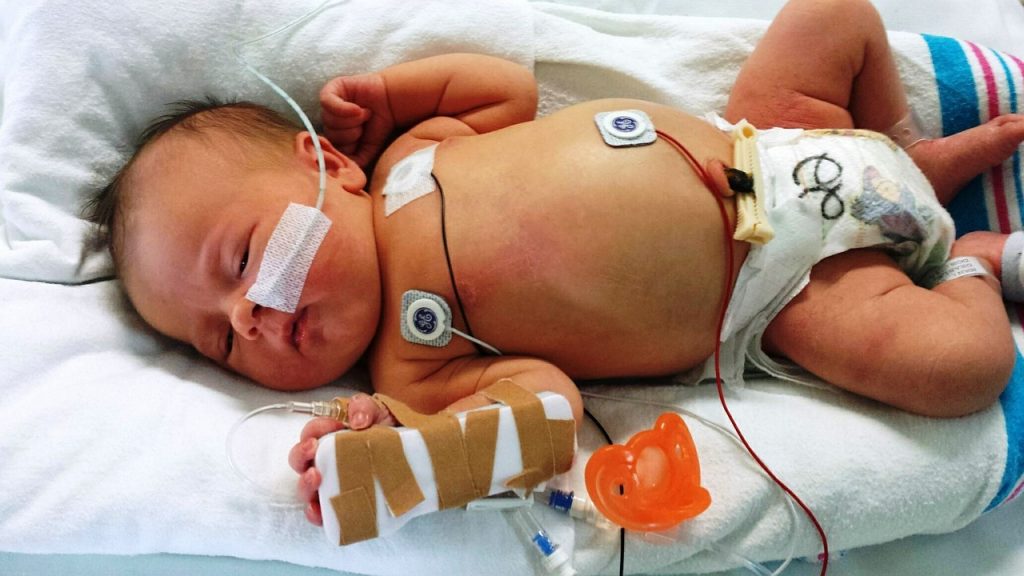
In the past few decades, physicians, nurses, hospitals, counselors, chaplains, and religious leaders have helped to extend the practices of palliative and hospice care to families of children with significantly life-limiting conditions. In our case, we were able to craft a novel form of care known as perinatal palliative and hospice care. This form of care enabled us to ease Sam’s discomfort during his short life after birth. We pursued a plan of non-aggressive care, including oxygen support with nasal cannula and palliative medicine for pain. The physicians and the nurses involved in our care enabled us to spend five sacred hours with Sam. Although his breathing was labored, the medication he received helped to ease his suffering. I do not doubt that his experience would have been much more difficult if he had not received this kind of care. I do not doubt that the experience of watching him die would have been much more difficult. I do not doubt that he would have suffered more than he did. But he received a kind of care that eased this burden even as he died.
I know something of the suffering Comstock has experienced. And I understand why he has been drawn to advocate approaches that would enable parents to ease their children’s suffering quickly and painlessly. I also understand how his proposal would protect parents from the difficulty of watching their children suffer as they die—an experience more difficult than I can communicate. But I reject the remedy he offers as a solution to this suffering. Active euthanasia is an act that aims at the death of a person—a person whose value is not dependent on his abilities or his capacities. Even if the act is motivated by the desire to ease pain, it does so by destroying the life of the sufferer. Killing a terminally ill child is not a mode of caring for the child.
And the suffering produced by these kinds of tragic circumstances is not a reason to abandon the moral distinction between killing and letting die; it is not a sufficient ground justifying the practice of active euthanasia. Rather, it is a reason to reaffirm the importance of caring for those who are dying by bringing the best of palliative medicine to bear on their needs. Medicine limps in the face of inevitable death, but it doesn’t follow that we should put our technical capacities to use in aiming at the death of our loved ones. Instead, we should put our abilities to use in seeking ways to care for them even as they die. Perinatal palliative and hospice care is an exemplary model of this form of care for families who receive an in-utero diagnosis of a significantly life-limiting condition. Families in these circumstances would be better served if the medical community and our public institutions found ways to increase access to these kinds of needful care.
Aaron D. Cobb is an associate professor of philosophy at Auburn University at Montgomery. He is the author of Loving Samuel: Suffering, Dependence, and the Calling of Love.