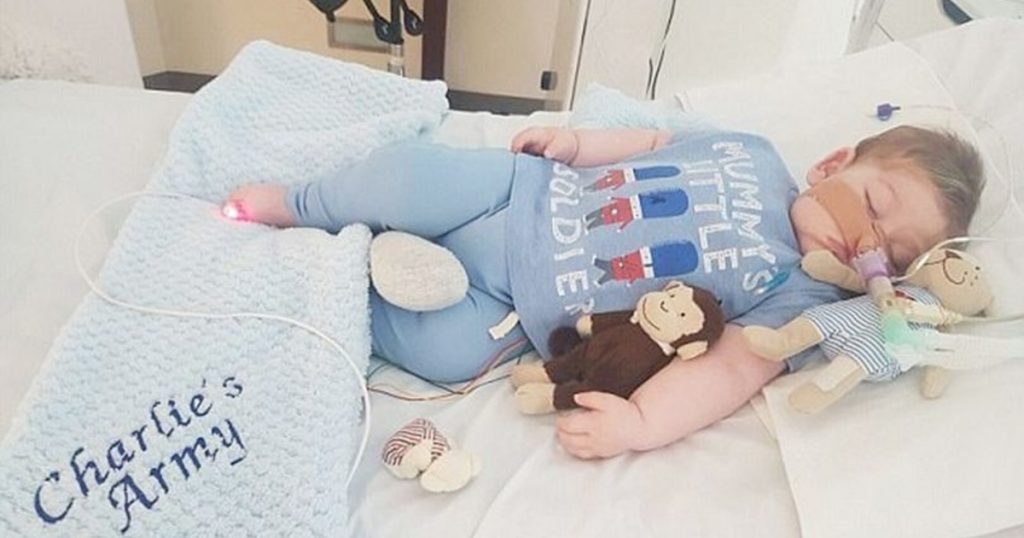
Much ink has been spilled debating whether or not further experimental treatment would be in the best interests of Charlie Gard. That debate is important and worthwhile. But it is not, in fact, the central question at issue in this case. Rather, the central question is: Who has the authority to make this controversial medical decision on Charlie’s behalf? The doctors at Ormond Street Hospital? The British courts? Or Charlie’s parents?
All three parties have some legitimate stake in the case. Like all medical professionals, Charlie’s doctors have the right to refuse to provide medical treatment to which they have a conscientious objection. Therefore, if they believe that further treatment for Charlie’s rare mitochondrial disorder would be unethical because his condition has deteriorated to the point at which it would only prolong Charlie’s suffering, they should not be forced to provide it. Yet in this case the British doctors are not only refusing to provide the requested treatment themselves; they also are seeking to prevent Charlie from receiving treatment from other doctors willing to provide it. They had no real right, therefore—at least from an ethical rather than legal perspective—to take the issue to court in the first place.
The state is charged with promoting the public good, which includes a responsibility to protect children from abuse and neglect. Yet giving further treatment to Charlie Gard presents no direct threat to the public good—not even economically, since the parents have raised the funds to pay for the treatment. Further, there is no question here of abuse or neglect. Indeed, the High Court went out of its way to praise Charlie’s parents, Connie Yates and Chris Gard, for their exceptional commitment and devotion to their son.
That leaves us with the parents. For the British doctors, Charlie is one among hundreds of patients—obviously a very special patient due to the rarity of the case and the public attention it has received, but nonetheless still one among many. For the United Kingdom, Charlie is just one of the millions of children within its realm. But for Connie and Chris, Charlie is a beloved son, with whom they have a unique, permanent, and irreplaceable bond. Connie and Chris gave Charlie his life and his identity. They are the ones who brought Charlie into the world, the ones to whom he is most intimately connected, and the ones most deeply invested in Charlie’s well-being. They are, therefore, the ones most directly responsible for Charlie’s care, and the ones with primary authority to make decisions on Charlie’s behalf.
Start your day with Public Discourse
Sign up and get our daily essays sent straight to your inbox.That the family (recognized as a natural pre-political community by great figures ranging from Aristotle and Locke to Gandhi and Confucius) possesses the right to a certain autonomy over its internal affairs is widely accepted not only as a matter of moral principle (as I have argued in previous articles and in a book), but also in national and international law. This right has been affirmed by the United States Supreme Court in cases like Meyer v. Nebraska, Pierce v. Society of Sisters, and Wisconsin v. Yoder. These cases all affirm the right of parents to direct the education and upbringing of their children as a fundamental aspect of a free society. This same basic principle applies to medical decision-making as well.
Similarly, Article 8 of the European Convention of Human Rights and Article 12 of the Universal Declaration Human Rights mark out the family as a private sphere that is relatively autonomous from coercive state interference, to the extent that that is compatible with the rights of others and the maintenance of a democratic society. The Universal Declaration further states that the family is “the natural and fundamental group unit of society” (Article 16) and that “parents have a prior right to choose the kind of education that shall be given to their children” (Article 26), again pointing to a broader principle of parental decision-making authority.
By using its coercive power to prevent Charlie from receiving further medical treatment, the United Kingdom is clearly overstepping the bounds of its legitimate authority, violating the right of Connie Yates and Chris Gard to make a profoundly intimate and important family decision about how best to care for their sick child.
But what about Charlie? Isn’t it justified for the state to step in order to prevent him from being subjected to additional pain and suffering, all for a slim hope of a slight improvement in his condition? Although no one doubts Charlie’s parents’ good intentions, might not prolonging his suffering on the basis of such faint and limited hope be nonetheless tantamount to abuse?
If it were clear that Charlie was suffering terribly and that further treatment would only exacerbate that suffering, then perhaps the answer would be yes, and state intervention would be justified. Nonetheless, the perhaps needs to be emphasized, especially because even when doctors are completely sure of their prognosis, they can nonetheless be wrong. Just consider the case of Jahi McMath, declared dead on neurological grounds by several expert doctors in California. Jahi’s parents disagreed with the doctors and had Jahi moved to a New Jersey facility that agreed to keep her on life support. Subsequent reports indicate that, while still extremely sick and disabled, Jahi is now uncontroversially alive and even able to make voluntary movements in response to her mother’s commands.
The case of Charlie Gard is far from crystal clear. The doctors have admitted that they are not sure whether, or to what extent, Charlie is in fact suffering. Nor are they sure whether, or to what extent, the experimental treatment will cause him suffering. Charlie’s mother insists that he is not in pain, adding “I promise everyone I would not sit there and watch my son in pain and suffering, I couldn’t do it.” Further, there is disagreement among medical expertsl about whether or not the experimental treatment will improve his state. The treatment has helped children with other variants of the disease, but the fact is that it has never yet been tried on someone with Charlie’s exact condition.
Given that reasonable and well-informed people who genuinely seek to promote Charlie’s well-being can and do disagree about whether or not pursuing the treatment is in Charlie’s best interests, it is absurd to consider the treatment a form of unintentional abuse. In this case, the courts are simply substituting their own controversial and uncertain judgment for that of the parents. And since there is frequently a fair amount of uncertainty and controversy in medical decision-making, the court’s intrusion in this case sets a precedent for extremely broad state interference with parents’ decisions regarding the medical care of their children. Even further, it sets a precedent for state intrusion in all medical decision-making.
For the right of parents to make medical decisions on behalf of their children is, in a certain respect, an aspect of the more general right of patients to make autonomous decisions about their own care. Imagine that Charlie was an adult suffering from terminal cancer, and that—directly, through a living will, or through a proxy—he indicated his wish to receive any and all possible life-prolonging treatments, even if they were painful, and even if they held out only a tiny hope of benefit. Imagine further that Charlie had the resources to pay for this treatment himself. In such a case, Charlie’s wishes would be followed. Some doctors might refuse to administer a treatment that they considered futile, but no one would take Charlie (or his proxy) to court to prevent him from receiving the treatment from another doctor. And even if someone did bring such a case to court, the judges would certainly rule in Charlie’s favor.
Of course, the real Charlie Gard is a baby and cannot make medical decisions for himself, appoint a proxy, or express his wishes in any way. But this is sometimes the case with adults as well. The documentary Extremis, which is a thought-provoking exploration of end-of-life decision-making, presents the case of a ventilator-dependent middle-aged woman who had suffered a traumatic brain injury. She appeared to be completely unresponsive, and there were no signs that her condition was improving. The woman had not written a will and had never explicitly indicated her wishes for end-of-life treatment. While the doctor believed that continuing life support was futile and recommended withdrawing it, the woman’s daughter, her closest relative and therefore the default health care proxy, felt that withdrawing the ventilator would be tantamount to killing her mother. I believe that the daughter was mistaken on this point; the choice to withdraw a disproportionately burdensome treatment is not a choice to kill someone, but rather a choice to avoid the burdens of the treatment, while accepting as an unintended side effect that the patient may die sooner as a result. Nonetheless, the doctor rightly followed the daughter’s wishes, because the daughter was the one with the authority to make the decision. The patient did unexpectedly have brief periods of consciousness before finally passing away several months later.
Thus, as in the case portrayed in Extremis, in the case of Charlie Gard the wishes of Charlie’s parents, the ones who have primary authority to make decisions on his behalf, should have been followed without further controversy. They should have been allowed to bring Charlie to the US for experimental treatment as soon as they had decided on that course of action. Perhaps the silver lining for Charlie and his parents is that, as a result of the media coverage and widespread public outrage, the US doctors are now offering to send the experimental drugs to the UK so that Charlie can receive the experimental treatment without having to endure transatlantic travel. Whether or not the British government will allow this to happen remains to be seen.
For the rest of us, perhaps the silver lining in this tragic case will be an increased public awareness of the need to be vigilant in defending parental decision-making authority against the encroachments of an overweening state.